Update (June 21, 2021): Healthcare providers receiving Provider Relief Fund payments will have to report to the government on using such payments before certain newly announced spending deadlines. The first spending deadline is June 30, 2021, with a 90-day reporting period beginning July 1, 2021, to report on funds received in the first half of 2020. For the most recent updates on future deadlines and further guidance on Provider Relief Fund reporting, visit our Provider Relief Fund reporting page.
Update: On Oct. 1, 2020, the U.S. Department of Health and Human Services, through the Health Resources and Services Administrative (HRSA), announced $20 billion in new Phase 3 General Distribution Funding for providers from the Public Health and Social Services Emergency Fund (Provider Relief Fund). For more information, please see our Oct. 2, 2020, alert.
Update (July 20, 2020): On July 17, 2020 the Department of Health and Human Services (HHS) announced that distribution of the second round of funding for high COVID-19 admission hospitals will begin during the week of July 20, 2020. More Information about this distribution is included in a July 20, 2020 McGuireWoods alert.
Update (July 13, 2020): On July 10, 2020, the Department of Health and Human Services (HHS) distributed an additional $1 billion to certain rural providers under the program discussed in this article. More information about this expansion is included in a July 12 McGuireWoods alert.
Update (June 10, 2020): HHS announced a second round of targeted funding for hospitals with high COVID-19 admissions. Hospitals have until June 15 to apply as discussed in a June 10, 2020 alert.
Update (May 22, 2020): Eligible providers have until June 3, 2020, to take action to be eligible to receive an additional payment from the Provider Relief Fund General Distribution, as discussed in a May 22, 2020 alert, which also discusses updated guidance.
Update (May 8, 2020): HHS provided updated information regarding the payment allocation methodology used in connection with the $12 billion COVID-19 high impact payments made to hospitals.
On May 1, 2020, HHS announced the release of $22 billion of the $100 billion public health and social services emergency fund (Provider Relief Fund) appropriated in the Coronavirus Aid, Relief, and Economic Security Act (CARES Act). The Provider Relief Fund was created to reimburse providers for healthcare-related expenses and lost revenue attributable to the 2019 novel coronavirus (COVID-19) pandemic.
As discussed in previous McGuireWoods legal alerts, $50 billion of the provider relief fund was allocated for general distribution to Medicare facilities and providers impacted by COVID-19. This newly announced $22 billion distribution targets hospitals with high COVID-19 admissions and rural providers.
High COVID-19 Admission Hospitals
HHS announced that each of 395 hospitals would receive a portion of $12 billion via direct deposit in the coming days. HHS stated that it utilized a simple formula to allocate and pay $10 billion through a fixed amount based on COVID-19 inpatient admission, while an additional $2 billion took into account the various hospitals’ Medicare and Medicaid disproportionate share and uncompensated care. This latter payment, previously unannounced, was made from the Provider Relief Fund for a total payment of $12 billion to hospitals with significant COVID-19 admissions.
While HHS did not disclose which hospitals would receive the funds, hospitals were required to apply through HHS’ COVID-19 portal before 3 p.m. (ET) on April 25, 2020. HHS also noted that each recipient hospital treated at least 100 COVID-19 inpatients as of April 10, 2020, and together represented 71 percent of reported admissions to HHS. Unsurprisingly, HHS’ geographic information suggests these funds were paid to hard-hit metropolitan areas with the most COVID-19 patients to date. For example, of the top U.S. counties receiving a portion of $2 billion in funds based on low-income and uninsured patients (described above), the five counties making up New York City were within the top six counties (with Cook County, surrounding Chicago, rounding out the six as third-highest). The remaining top 10 counties surround Los Angeles, Miami, Indianapolis and Boston. The national distribution of this full allocation for high COVID-19 admission hospital payment similarly shows significant funding for states with hard-hit metropolitan areas, including New York City, Detroit, Chicago, Boston and New Orleans.
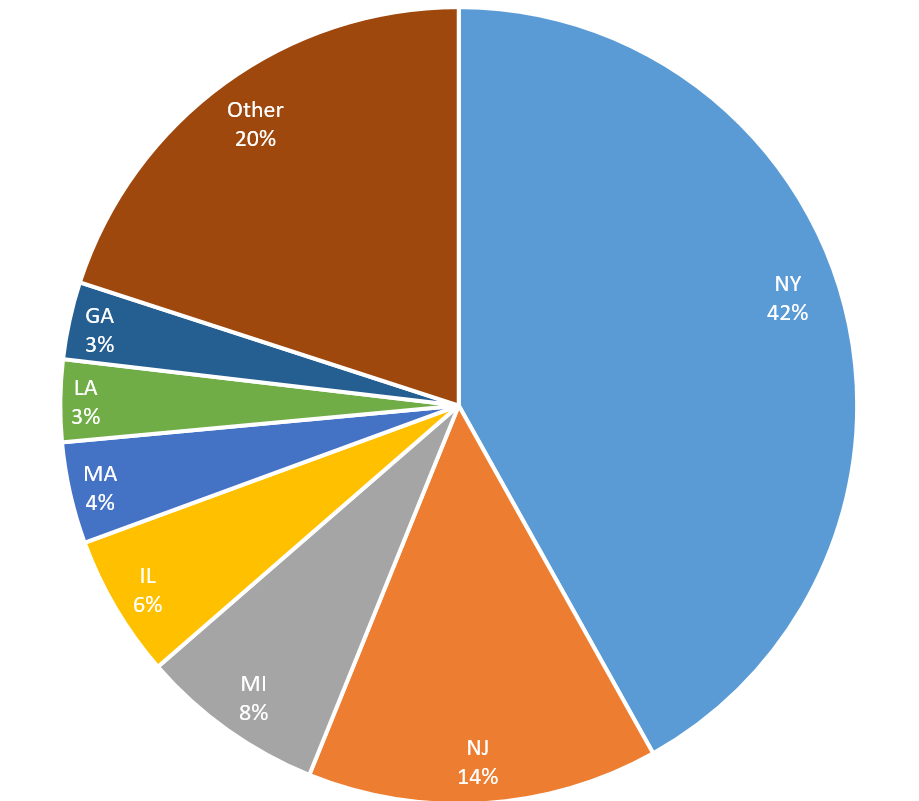
HHS made these targeted distributions to assist hospitals because “inpatient admissions are a primary driver of costs to hospitals related to COVID-19.” Notably, hospitals will also have access to Medicare add-on payment for inpatient COVID-19 admissions included in the CARES Act, as discussed in a prior McGuireWoods legal alert.
Rural Providers
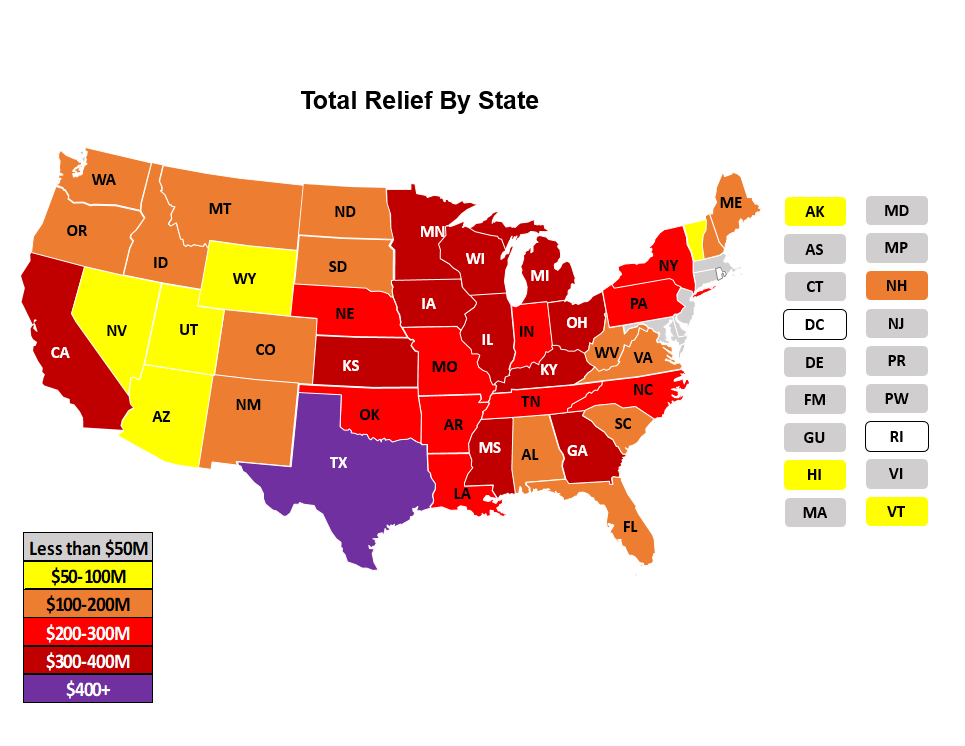
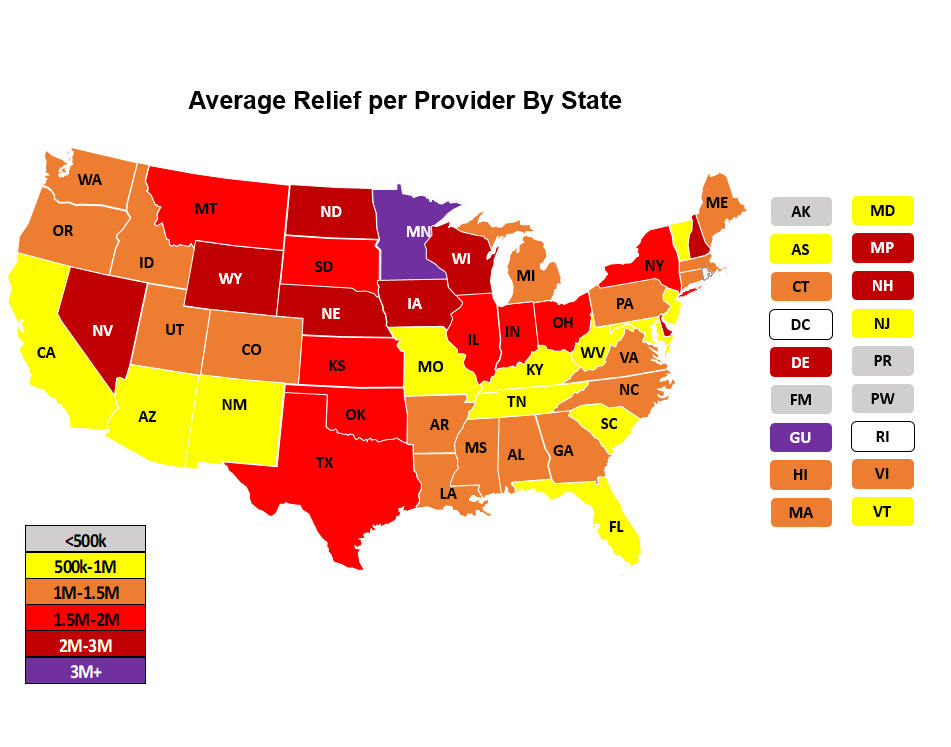
HHS also announced payment of $10 billion targeted to rural providers via direct deposits, based on operating expenses. These payments were to be made to acute care general hospitals, critical access hospitals (CAH), rural health clinics (RHC) and community health centers (CHC) located in rural areas. As demonstrated by the two maps below (the map on the left with total amounts paid to providers in each state, and the map on the right with the average amount paid to providers in each state), funding to states reached a broader base of providers than did the distribution to the 395 hospitals, with less significant geographic concentration as in the previously described grant.
Click each map to open an expanded view.
Much as it did for the hospital distribution, HHS stated that it intended to utilize a simple formula for its distribution to rural providers. Specifically, HHS calculated a minimum base payment for these rural providers plus a percent of their annual expenses, assuming this information was available to HHS. For RHCs with no reported Medicare claims and CHCs lacking expense data, HHS will provide a $100,000 base payment. Similarly, rural acute care general hospitals and CAHs will receive a $1 million base payment. In both cases, additional payments based on annual expenses will be made, although HHS did not provide background on this formula.
HHS made this targeted distribution to assist rural providers, acknowledging that many were operating on thin margins prior to the COVID-19 pandemic. Like providers in urban settings, rural providers have also faced elective procedure delays and cancellations affecting their financial backing while, at the same time, having to prepare for any community COVID-19 surges.
* * * * *
Recipients of the targeted hospital and rural provider distributions remain eligible for general distributions from the Provider Relief Fund, including the second-round $20 billion funding that began April 24, 2020. As discussed in a prior McGuireWoods legal alert, such providers may have received a portion of this second general distribution if they submit Medicare cost reports. If such funds were not received automatically, the provider can apply through a web portal.
Further, as part of its discussion of the distribution to high COVID-19 admission hospitals and rural providers, HHS reiterated that it plans to target distributions to other providers, including but not limited to skilled nursing facilities, dentists and providers that solely take Medicaid. Additionally, HHS will reimburse providers for testing and treating uninsured COVID-19 patients; they can now sign up for this funding, as discussed in this prior McGuireWoods legal alert. These funds are provided through the CARES Act as supplemented by $75 billion in the Paycheck Protection and Healthcare Enhancement Act. (More information is available in an April 23, 2020, McGuireWoods legal alert.)
HHS continues to release details on these funds, and McGuireWoods continues to monitor all information released by HHS and the Trump administration regarding the same. Please contact the authors or any of the McGuireWoods COVID-19 Response Team members for additional information on the Provider Relief Fund and its availability to healthcare providers and for assistance with the documentation and reporting process.
 |
COVID-19: Healthcare Video AlertsIn a series of video alerts, McGuireWoods’ healthcare lawyers address issues providers face and overcoming COVID-19 challenges. |